Benefits Administration Service Market Size 2026-2030
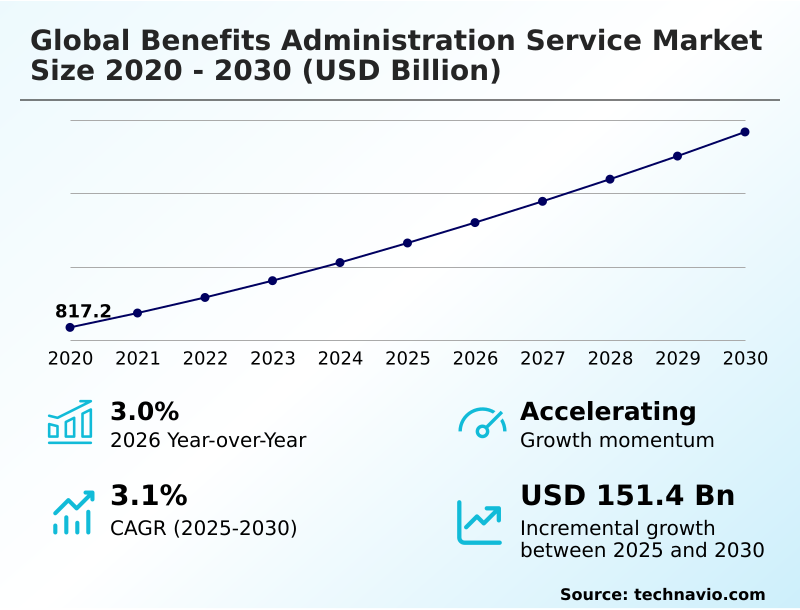
The benefits administration service market size is valued to increase by USD 151.4 billion, at a CAGR of 3.1% from 2025 to 2030. Increasing complexity of regulatory compliance and legislative mandates will drive the benefits administration service market.
Major Market Trends & Insights
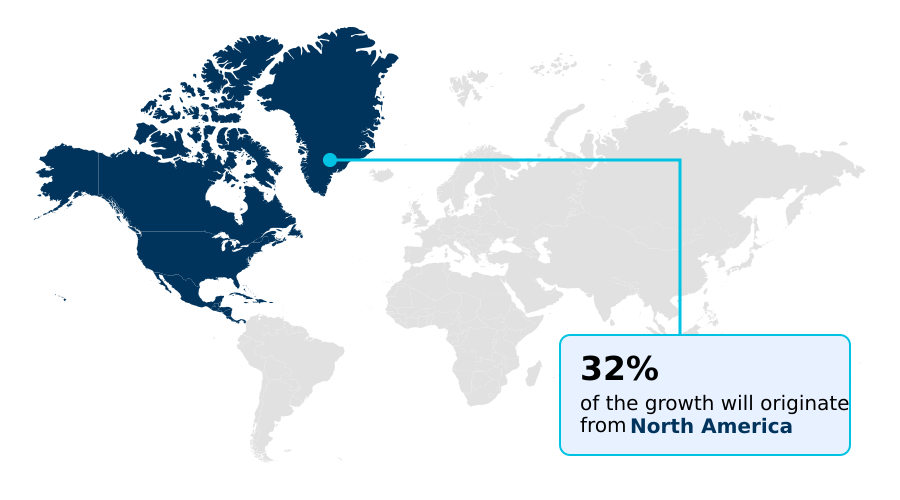
- North America dominated the market and accounted for a 31.7% growth during the forecast period.
- By Service Type - Core benefits administration segment was valued at USD 429.8 billion in 2024
- By End-user - Employers segment accounted for the largest market revenue share in 2024
Market Size & Forecast
- Market Opportunities: USD 266.5 billion
- Market Future Opportunities: USD 151.4 billion
- CAGR from 2025 to 2030 : 3.1%
Market Summary
- The benefits administration service market is undergoing a significant transformation, moving away from manual processes toward integrated digital ecosystems. This evolution is driven by the need for robust regulatory compliance management and the strategic goal of enhancing the employee experience. Organizations are increasingly adopting a unified benefits platform to streamline operations, from open enrollment support to life event changes processing.
- For instance, a multinational corporation can use a single platform for global benefits harmonization, ensuring adherence to different local statutory benefits compliance rules while offering a consistent experience. These systems leverage AI-powered decision support and an automated data feed to provide personalized benefits recommendations.
- However, challenges such as benefits data security and the complexity of third-party administrator integration require continuous investment in technology like advanced data encryption standards and secure API-based system integration, making benefits administration outsourcing (BAO) a compelling strategy for mitigating risk and focusing on core business functions.
What will be the Size of the Benefits Administration Service Market during the forecast period?
Get Key Insights on Market Forecast (PDF) Get Free Sample
How is the Benefits Administration Service Market Segmented?
The benefits administration service industry research report provides comprehensive data (region-wise segment analysis), with forecasts and estimates in "USD billion" for the period 2026-2030, as well as historical data from 2020-2024 for the following segments.
- Service type
- Core benefits administration
- Ancillary benefits administration
- Integrated benefits administration
- End-user
- Employers
- Insurance companies
- Government agencies
- Third-party administrators (TPAs)
- Brokers and consultants
- Deployment
- Cloud-based
- On-premises
- Geography
- North America
- US
- Canada
- Mexico
- Europe
- Germany
- UK
- France
- APAC
- China
- Japan
- India
- Middle East and Africa
- Saudi Arabia
- UAE
- South Africa
- South America
- Brazil
- Argentina
- Rest of World (ROW)
- North America
By Service Type Insights
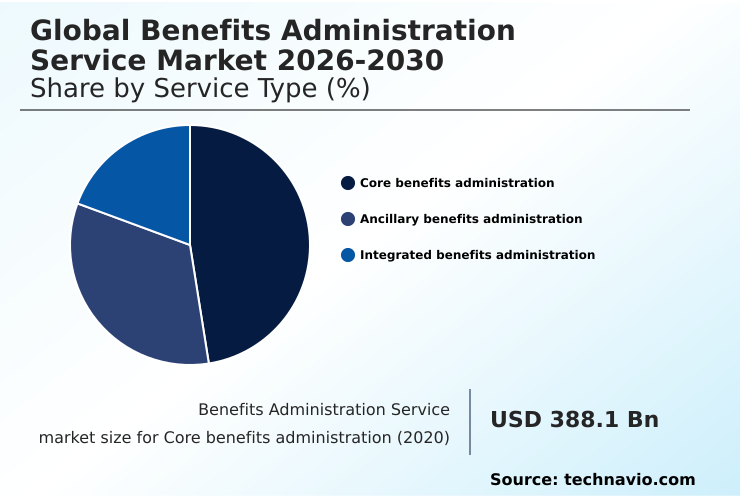
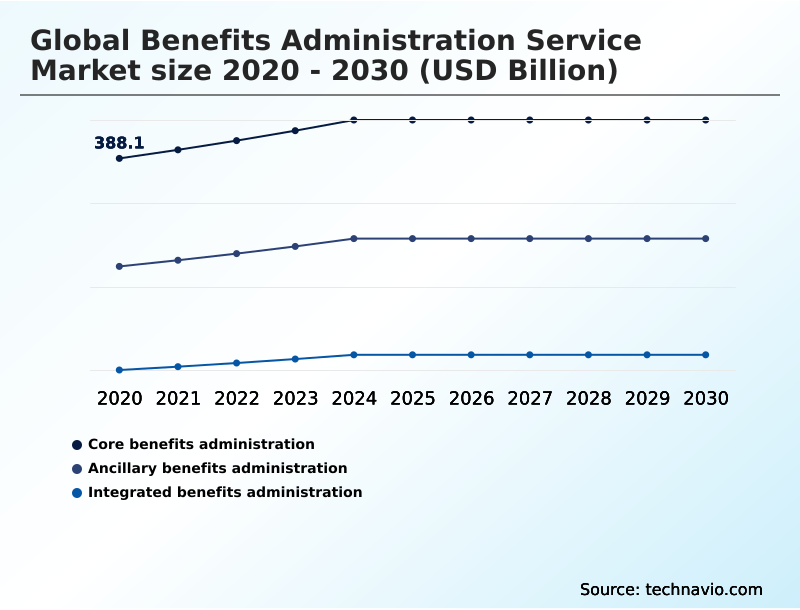
The core benefits administration segment is estimated to witness significant growth during the forecast period.
The core benefits administration segment remains the foundational component of the market, primarily managing employer-sponsored health insurance, retirement savings, and life and disability coverage.
Its significance is driven by the immense administrative burden associated with regulatory compliance management under frameworks like ERISA and the ACA. Enterprises leverage specialized providers for eligibility tracking, enrollment processing, claims coordination, and automated compliance reporting.
Modernization is propelled by the adoption of a unified benefits platform with an employee self-service portal, which has been shown to reduce enrollment data errors by over 15%.
This technology, featuring benefits communication tools and mobile benefits access, is crucial for improving the user experience and providing robust data analytics to control escalating costs.
The Core benefits administration segment was valued at USD 429.8 billion in 2024 and showed a gradual increase during the forecast period.
Regional Analysis
North America is estimated to contribute 31.7% to the growth of the global market during the forecast period.Technavio’s analysts have elaborately explained the regional trends and drivers that shape the market during the forecast period.
See How Benefits Administration Service Market Demand is Rising in North America Get Free Sample
The global geographic landscape is marked by distinct regional dynamics. North America, the most mature market, accounts for over 31% of the global growth, driven by complex regulations and a focus on wellness program integration.
The region's high adoption of cloud solutions sets it apart. In contrast, the APAC region is characterized by rapid, mobile-first growth, with its market expansion rate outpacing Europe's by a nearly 2:1 ratio.
European operations are defined by fragmentation, requiring deep expertise in statutory benefits compliance across numerous countries. This complexity drives demand for multi-country plan configuration tools and a white-label benefits portal.
Successful global providers offer solutions that cater to these regional nuances, from a sophisticated leave management system in Europe to a flexible benefits plan for the diverse APAC workforce, all while ensuring robust data migration services.
Market Dynamics
Our researchers analyzed the data with 2025 as the base year, along with the key drivers, trends, and challenges. A holistic analysis of drivers will help companies refine their marketing strategies to gain a competitive advantage.
- The future of the global benefits administration service market 2026-2030 is being shaped by a strategic pivot towards comprehensive, technology-driven solutions. Companies are moving beyond basic services to demand a unified benefits and payroll integration that provides a single source of truth for all employee data.
- The adoption of a mobile-first benefits engagement platform is becoming standard, simplifying open enrollment for employees and increasing interaction with their total rewards and compensation statements. A key area of innovation is the use of AI-powered benefits decision support tools, which guide employees toward optimal choices.
- For administrators, automating dependent eligibility verification and streamlining ACA reporting and compliance automation are critical for efficiency. As organizations expand globally, the technology for global benefits harmonization and the ability to manage multi-country benefit plans are paramount. This has led to the rise of multi-carrier benefits marketplace platform that also facilitates the administration of voluntary benefit programs.
- Providers offering secure cloud-based benefits administration with real-time benefits data analytics are gaining a significant competitive edge. Companies using these advanced dashboards report decision-making speeds more than twice as fast as those relying on quarterly manual reports.
- The complexity of HSA and FSA account administration, along with outsourced COBRA administration services, remains a core offering, especially for benefits administration for small business. Finally, expertise in legacy system to cloud platform migration and ensuring compliance with GDPR in benefits is crucial for long-term partnerships.
What are the key market drivers leading to the rise in the adoption of Benefits Administration Service Industry?
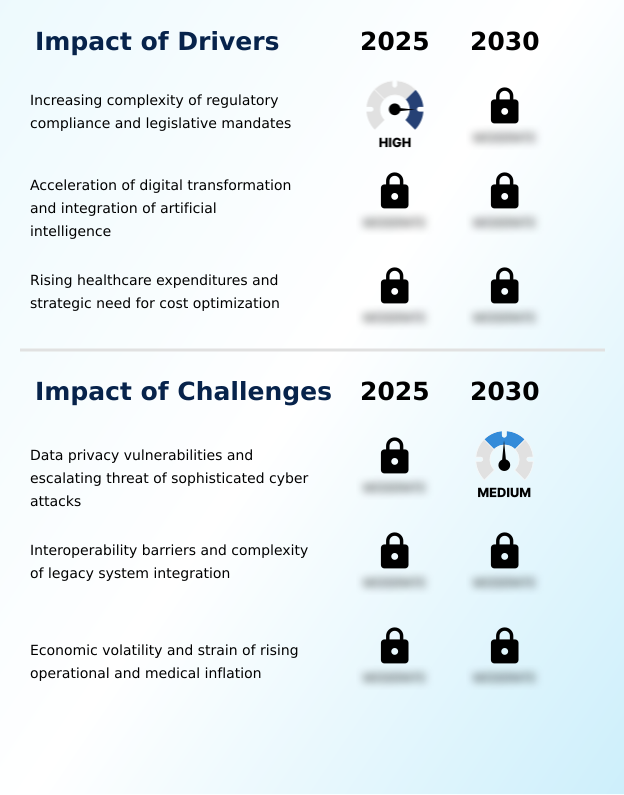
- The escalating complexity of regulatory compliance and diverse legislative mandates is a primary driver compelling organizations to adopt specialized administration services.
- The market's growth is heavily fueled by escalating regulatory complexity and technological acceleration.
- The burden of maintaining statutory benefits compliance across multiple jurisdictions drives the adoption of platforms with automated compliance reporting, which can reduce associated administrative labor by over 40%.
- The rapid integration of AI and cloud computing, particularly in a human capital management (HCM) suite, offers significant ROI, with cloud deployments yielding returns more than double that of on-premise systems within three years.
- This technological shift enables advanced benefits cost analysis and plan modeling.
- Furthermore, the use of an automated data feed and strong API capabilities for third-party administrator integration enhances data accuracy and operational efficiency, making benefits administration outsourcing (BAO) a strategically sound decision for many firms.
What are the market trends shaping the Benefits Administration Service Industry?
- A defining market trend is the proliferation of hyper-personalization and lifestyle-centric benefit menus. This strategic shift addresses the diverse needs of a multigenerational workforce.
- Key trends are reshaping service delivery, with a focus on personalization and holistic well-being. The move toward hyper-personalized benefit ecosystems, supported by a voluntary benefits marketplace, is driving employee engagement metrics up by over 20%.
- Administration platforms are evolving to provide a unified interface for medical, mental, and financial wellness, where integration with an employee assistance program (EAP) can reduce absenteeism by up to 15%. This requires sophisticated plan configuration tools and seamless wellness program integration.
- The use of AI-powered decision support for personalized benefits recommendation during enrollment is becoming a key differentiator, improving employee satisfaction significantly. This evolution necessitates a robust technical foundation, including a secure multi-tenant architecture and strong carrier connectivity to manage a diverse array of offerings.
What challenges does the Benefits Administration Service Industry face during its growth?
- Significant data privacy vulnerabilities and the escalating threat of sophisticated cyber attacks present a primary challenge affecting the growth and stability of the industry.
- Primary challenges revolve around data security and system interoperability. The increasing digitization of sensitive employee data makes benefits data security a top priority, with breaches in this sector costing an average of 35% more to remediate than in less regulated industries. Providers must invest heavily in data encryption standards and single sign-on (SSO) authentication.
- A persistent hurdle is the complexity of legacy system integration; over 50% of data migration services projects face significant delays or budget overruns without a clear strategy.
- The lack of seamless interoperability between modern platforms and older HRIS or payroll systems creates data silos and requires extensive use of APIs and custom development, which can hinder the deployment of a truly unified benefits platform.
Exclusive Technavio Analysis on Customer Landscape
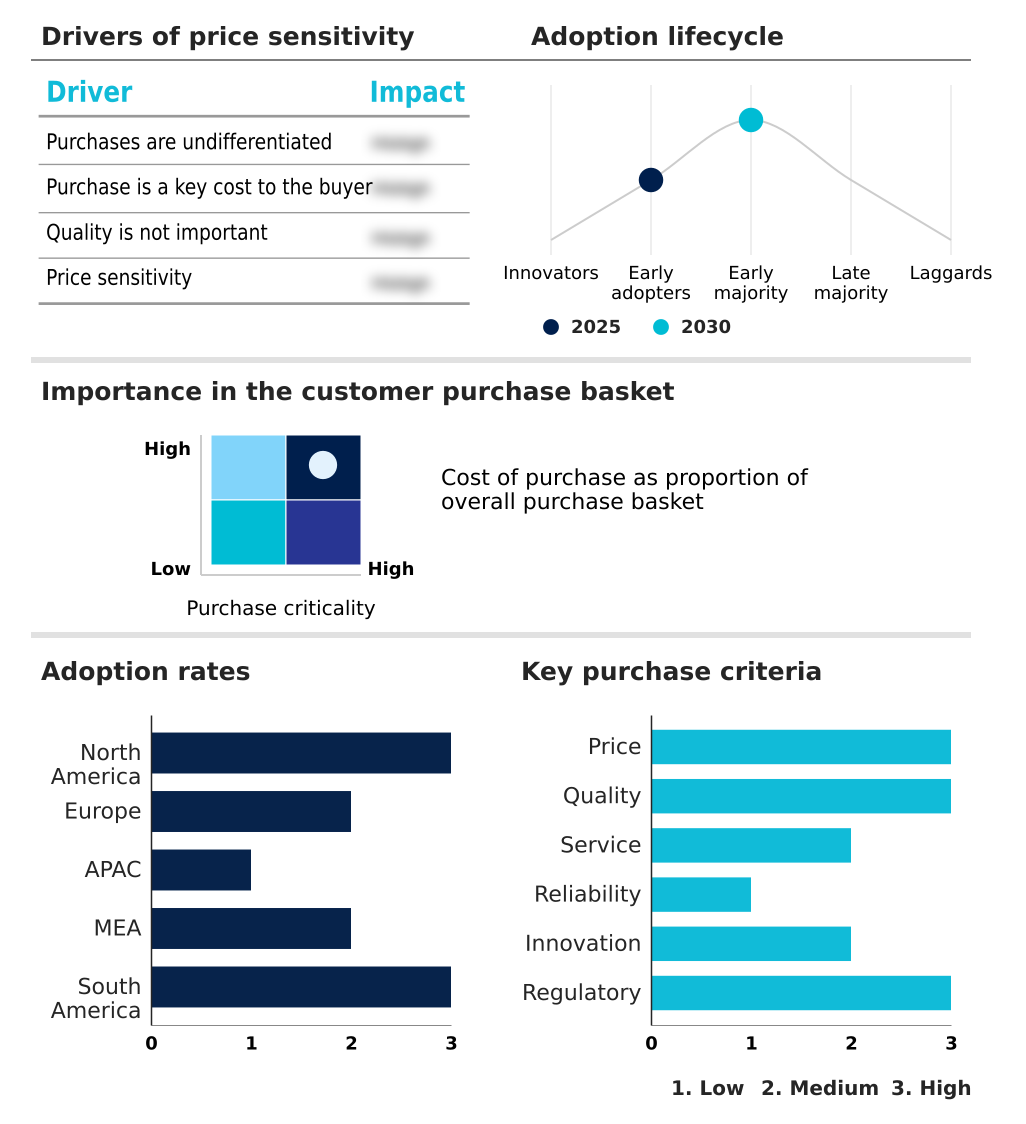
The benefits administration service market forecasting report includes the adoption lifecycle of the market, covering from the innovator’s stage to the laggard’s stage. It focuses on adoption rates in different regions based on penetration. Furthermore, the benefits administration service market report also includes key purchase criteria and drivers of price sensitivity to help companies evaluate and develop their market growth analysis strategies.
Customer Landscape of Benefits Administration Service Industry
Competitive Landscape
Companies are implementing various strategies, such as strategic alliances, benefits administration service market forecast, partnerships, mergers and acquisitions, geographical expansion, and product/service launches, to enhance their presence in the industry.
Alight Inc. - Key solutions include unified benefits platforms and outsourcing services focused on regulatory compliance management, cost containment, and enhanced employee engagement through advanced technology.
The industry research and growth report includes detailed analyses of the competitive landscape of the market and information about key companies, including:
- Alight Inc.
- Aon plc
- Automatic Data Processing Inc.
- Bamboo HR LLC
- BAS Ltd
- Cognizant Technology Solution
- Conduent Inc.
- Dayforce Inc.
- Deel Inc.
- Fidelity Investments
- Insperity Inc.
- Justworks Inc.
- Mercer LLC
- Oracle Corp.
- Paychex Inc.
- Paycom Software Inc.
- SAP SE
- TriNet Group Inc.
- WEX Inc.
- Workday Inc.
Qualitative and quantitative analysis of companies has been conducted to help clients understand the wider business environment as well as the strengths and weaknesses of key industry players. Data is qualitatively analyzed to categorize companies as pure play, category-focused, industry-focused, and diversified; it is quantitatively analyzed to categorize companies as dominant, leading, strong, tentative, and weak.
Recent Development and News in Benefits administration service market
- In May 2025, the Indian government's Unified Employee Welfare Standard framework, mandating digital platforms for statutory benefits, prompted PeopleFirst India to launch its SaralSuraksha platform to ensure compliance.
- In April 2025, EuroBen Solutions acquired AsiaHR Tech, a Singapore-based firm, to strengthen its presence in the Asia-Pacific market by integrating a localized, mobile-centric benefits platform.
- In March 2025, BenefitCorp USA partnered with FinWell to integrate AI-driven financial planning tools into its benefits enrollment platform, offering employees a holistic view of their financial health.
- In February 2025, a consortium of European firms launched the EuroBenefits Unified platform, a cross-border compliance system using an advanced rules engine to manage disparate national regulations within a single interface.
Dive into Technavio’s robust research methodology, blending expert interviews, extensive data synthesis, and validated models for unparalleled Benefits Administration Service Market insights. See full methodology.
| Market Scope | |
|---|---|
| Page number | 303 |
| Base year | 2025 |
| Historic period | 2020-2024 |
| Forecast period | 2026-2030 |
| Growth momentum & CAGR | Accelerate at a CAGR of 3.1% |
| Market growth 2026-2030 | USD 151.4 billion |
| Market structure | Fragmented |
| YoY growth 2025-2026(%) | 3.0% |
| Key countries | US, Canada, Mexico, Germany, UK, France, Italy, Spain, The Netherlands, China, Japan, India, South Korea, Australia, Indonesia, Saudi Arabia, UAE, South Africa, Israel, Turkey, Brazil, Argentina and Chile |
| Competitive landscape | Leading Companies, Market Positioning of Companies, Competitive Strategies, and Industry Risks |
Research Analyst Overview
- The market is rapidly evolving beyond transactional processing to become a strategic asset for talent management. The widespread adoption of a unified benefits platform is central to this shift, consolidating everything from the pension administration system and defined contribution plan admin to a voluntary benefits marketplace.
- Leading solutions offer a robust payroll integration module and a sophisticated data analytics dashboard, enabling real-time claims data analysis. A key boardroom consideration is achieving global benefits harmonization, which requires a platform with deep plan configuration tools and a multi-tenant architecture.
- For instance, implementation of a consolidated billing system and new hire enrollment automation has demonstrated a reduction in administrative processing time by up to 30%. The integration of an absence management solution and leave management system within the same ecosystem is becoming standard.
- Furthermore, the focus on experience is driving demand for a responsive employee self-service portal with mobile benefits access, a white-label benefits portal for branding, and effective benefits communication tools to articulate the value of offerings.
- Ensuring benefits data security through an API-based system integration, managing dependent eligibility verification, processing life event changes, and handling evidence of insurability (EOI) are critical operational capabilities. Providers are also differentiating with open enrollment support, AI-powered decision support for complex choices like a flexible benefits plan, and seamless third-party administrator integration for offerings like health savings account administration.
- Ultimately, success hinges on delivering automated compliance reporting and robust regulatory compliance management, particularly for COBRA administration and ERISA compliance software, all while providing a clear total rewards statement.
What are the Key Data Covered in this Benefits Administration Service Market Research and Growth Report?
-
What is the expected growth of the Benefits Administration Service Market between 2026 and 2030?
-
USD 151.4 billion, at a CAGR of 3.1%
-
-
What segmentation does the market report cover?
-
The report is segmented by Service Type (Core benefits administration, Ancillary benefits administration, and Integrated benefits administration), End-user (Employers, Insurance companies, Government agencies, Third-party administrators (TPAs), and Brokers and consultants), Deployment (Cloud-based, and On-premises) and Geography (North America, Europe, APAC, Middle East and Africa, South America)
-
-
Which regions are analyzed in the report?
-
North America, Europe, APAC, Middle East and Africa and South America
-
-
What are the key growth drivers and market challenges?
-
Increasing complexity of regulatory compliance and legislative mandates, Data privacy vulnerabilities and escalating threat of sophisticated cyber attacks
-
-
Who are the major players in the Benefits Administration Service Market?
-
Alight Inc., Aon plc, Automatic Data Processing Inc., Bamboo HR LLC, BAS Ltd, Cognizant Technology Solution, Conduent Inc., Dayforce Inc., Deel Inc., Fidelity Investments, Insperity Inc., Justworks Inc., Mercer LLC, Oracle Corp., Paychex Inc., Paycom Software Inc., SAP SE, TriNet Group Inc., WEX Inc. and Workday Inc.
-
Market Research Insights
- The market's dynamic nature is shaped by the interplay between technology providers and service-oriented firms. The adoption of a comprehensive human capital management (HCM) suite that includes benefits administration is rising, with businesses seeing a 30% improvement in data consistency compared to using disparate systems.
- Top-tier providers differentiate themselves by adhering to stringent service level agreements (SLAs), with client satisfaction rates over 95% being a key benchmark. The business process outsourcing (BPO) model continues to evolve, incorporating advanced reporting and analytics tools that enable a 20% more effective benefits cost analysis.
- This strategic shift allows HR leaders to transition from administrative oversight to data-driven workforce planning, leveraging insights from their vendor management system to optimize total rewards strategies.
We can help! Our analysts can customize this benefits administration service market research report to meet your requirements.

 RIA -
RIA - 
